Inside the ICU
Critical care for lives in the balance
COVER STORY
By John Soeder
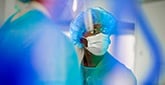
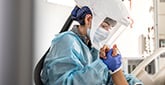
A nurse in the MICU gives medicine to a patient with COVID-19. | Photo: Annie O'Neill
The first thing you notice is an unexpected sense of calm. Yes, the care provided here is, by definition, intensive. But at this particular moment, the intensity is quietly focused.
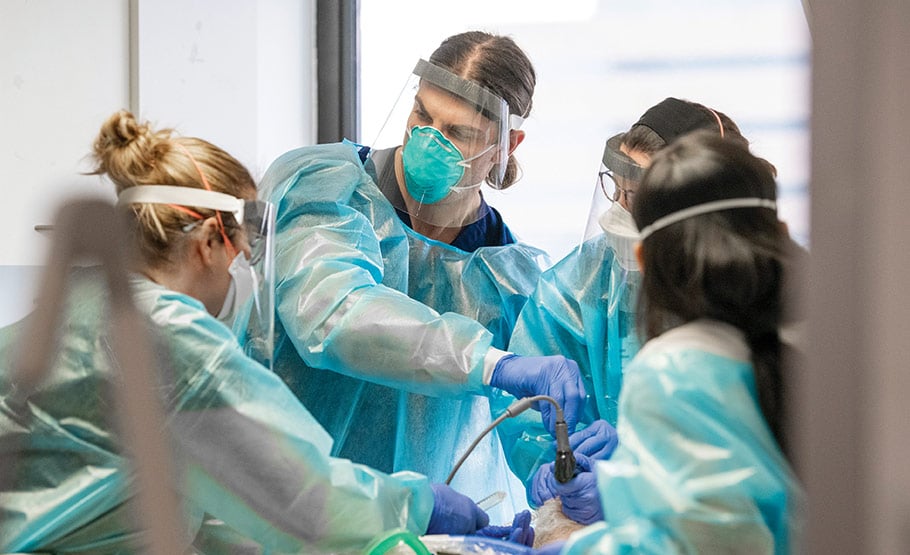
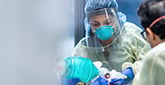
Dr. Patrick Lindsay, a critical care fellow (center), works with respiratory therapist Dawn Murphy (left) and Dr. Devora Lichtman (third from left) to intubate a patient. | Photo: Lisa DeJong
If this were a street corner, it would be the intersection of Life and Death. The gray light of a winter morning streams through the windows. Various monitors beep, buzz and chirp, like a field full of electronic crickets. Snatches of conversation can be overheard:
“Do you want me to wash your back for you?”
“You’re looking good! Your heart rate came down.”
“You call me if you need anything, OK?”
Eighteen beds line the perimeter; all but one is occupied. Some people are just passing through. Others will pass away.
All around them, an intricately choreographed ballet unfolds, subject to sudden bursts of urgent improvisation when things take a turn for the worse. Not if. When.
A team of caregivers is rounding, going from bedside to bedside for an in-depth update on each patient’s condition. It’s a flash mob of compassion.
In their personal protective equipment — face masks, face shields, disposable gowns and gloves — the physicians, nurses, respiratory therapists and other caregivers could pass for interplanetary travelers. Their workplace even looks like the deck of a spaceship, all sliding glass doors and gleaming white surfaces and cutting-edge technology tethered to humanity at its most fragile.
Here, machines do things that some bodies are too broken to do themselves, at least for now. Machines that breathe. Machines that pump blood. Machines that filter waste from the body. IV poles support networks of infusion pumps; some patients need as many as 15. And bedside monitors broadcast a colorful dashboard of vital signs and other body functions: the telemetries of lives hanging in the balance.
Welcome to the ICU.

Dr. Caroline Olt, an internal medicine resident, comforts the relative of a patient. | Photo: Annie O'Neill
Care Around the Clock
In the simplest terms, critical care is focused on caring for the sickest of the sick.
We’re talking about patients with life-threatening and frequently complex medical conditions, often involving vital organs such as the heart, lungs or liver. These patients typically find themselves in an intensive care unit, where they’re closely monitored and looked after around the clock by a multidisciplinary team of caregivers well-versed in specialized care and various modes of life support.
Critical care began to come into its own in the 1950s, when the modern ICU was developed amid the polio epidemic. Seven decades later, in the throes of another global health crisis, critical care is arguably more critical than ever.
“Because of the pandemic, people today are more familiar with critical care,” says Hassan Khouli, MD, Chair of the Department of Critical Care Medicine within Cleveland Clinic’s Respiratory Institute.
“It’s a relatively young specialty,” Dr. Khouli says. “It’s constantly evolving, too. At its foundation, you have dedicated caregivers from different disciplines working together to coordinate the care of critically ill patients 24/7.”
Across Cleveland Clinic’s health system as well as at other hospitals, separate intensive care units are dedicated to various subspecialties, including medical ICUs (MICUs), cardiovascular ICUs, neurological ICUs, neonatal ICUs, pediatric ICUs and surgical ICUs.
As Raed Dweik, MD, Chair of Cleveland Clinic’s Respiratory Institute, puts it: “Critical care comes in different flavors.”
With 64 beds across five nursing units, the MICU on Cleveland Clinic’s main campus is one of the largest and busiest in the United States. It has more than 4,500 admissions per year. Approximately 40% of patients arrive by way of the Emergency Department. Others come from other areas within Cleveland Clinic or via transfers from other hospitals across the region, from coast to coast and around the world.
“At Cleveland Clinic, our systemness is one of our greatest strengths,” Dr. Khouli says. “Our ICUs don’t operate in a silo or in a vacuum. We have the ability to coordinate across our different ICUs, leverage their strengths and share resources and best practices. We can move critically ill patients based on the ability of an ICU to meet their particular needs or — as we’ve seen with patients with COVID-19 — based on ICU capacity.”
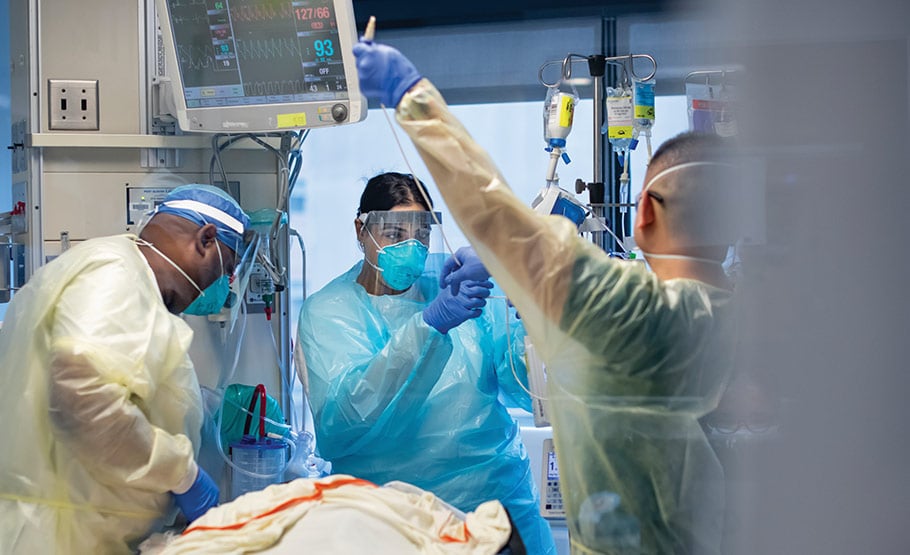
Nurse Amna Mustafa (center) confirms medication for a patient, joined by Nurse Timothy Washington (left) and Clinical Technician Jed Santo Domingo. | Photo: Annie O'Neill
It Takes a Team
When it comes to providing critical care, nothing is more critical than teamwork.
In the ICU, teams are led by critical care physicians, also known as intensivists. Nurses thoroughly assess patients and execute detailed care plans. Respiratory therapists are experts in managing ventilators. Teams may also include advanced practice providers, fellows, residents, occupational therapists, physical therapists and social workers, among others.
“Critical care is the ultimate team sport,” Dr. Dweik says. “We’re seeing teams continue to expand to address the complexities that come with critically ill patients.”
In recent years, pharmacists and dietitians also have been added to critical care teams. “They’re key team members,” Dr. Khouli says. “Having pharmacists rounding with the teams reduces medication errors in the ICU, where the pharmacology can get very complicated. It’s also a place where paying close attention to nutrition is extremely important, so having dietitians on the teams is invaluable.”
It takes a special breed to answer the call in an ICU.
“The camaraderie is undeniable,” says critical care nurse Stephanie Smith, RN, CCRN. “It’s akin to soldiers in battle. It feels like we’re in the trenches together, and we have each other’s backs.”
The work is stressful, even more so now in the time of COVID. The pace is fast and unforgiving. And the stakes couldn’t be higher.
“It’s a tough environment,” says Eduardo Mireles-Cabodevila, MD, Director of the MICU at Cleveland Clinic. “We try to keep patients as comfortable as possible, but they have to go through uncomfortable procedures. This is probably the most critical time in their lives. Either they’re nearing the end, or the course of their lives will change forever because they were in an intensive care unit.”
Nonetheless, there is no place Dr. Mireles-Cabodevila would rather be. He was a paramedic when he was still in high school in his native Mexico. Before he finished med school, he knew he wanted to be a critical care physician.
“This is my calling,” he says. “When people come to us, they’re very sick. They may have a high probability of dying, unless we can do something. Our job is to figure out what’s wrong, stabilize them and treat them, so hopefully they can recover and get on with the rest of their lives.”

“Critical care is the ultimate team sport. We’re seeing teams continue to expand to address the complexities that come with critically ill patients.”
— RAED DWEIK, MD | Chair of Cleveland Clinic’s Respiratory Institute

Nurse Assistant Christine Houston tends to a recently deceased patient. | Photo: Annie O'Neill
The Covid Years
Roughly two-thirds of the beds in Cleveland Clinic’s MICU are reserved for patients with COVID. At the height of the recent omicron surge, there were six straight weeks when every one of those beds was filled.
“It’s tough on us as caregivers,” says Dr. Mireles-Cabodevila. “Some people think, ‘Oh, they see this all the time; it doesn’t hurt.’ But it does. It takes a toll.”
Amid the pandemic, the sickest of the sick have become even sicker — and caring for them has become even more complicated, according to Smith.
“Before, if a patient hit their call button because they wanted their shoulder scratched, I could simply put foam on my hand, go in the room, scratch their shoulder, put foam on my hand and go back out,” she says. “Now, I have to do this whole routine and put on a mask and a gown whenever I enter the room, even if it’s just to scratch someone’s shoulder. I feel bad because I can’t always do the little things that I used to be able to do.”
How has COVID affected critical care? A better question might be: How hasn’t it?
“Early in the pandemic, there was a lot of information floating around, good, bad and everything in between,” Dr. Dweik says. “We focused on best practices — what to do, what not to do. We worked with the Education Institute to create COVID e-learning modules, which were viewed hundreds of thousands of times.”
Adi Gerblich, MD, of the Department of Critical Care Medicine developed an innovative platform that allows family members of patients to participate virtually in rounding (the ICU team’s daily check-in with patients) via video conference. “With limited visitation during the pandemic, patients can feel isolated,” Dr. Dweik says. “Families are an integral part of the care team, too, and this is a way to keep patients and families connected.”
More recently, critical care experts from Cleveland Clinic locations in the U.S. and abroad shared pandemic learnings in a virtual conference presented by Cleveland Clinic London.
“As a global health system, Cleveland Clinic has a big advantage,” Dr. Khouli says. “We can learn from our colleagues around the globe, and share our knowledge and best practices with them. The more data you have, the better you can identify trends and make adjustments that will help patients, whether they’re in Ohio or Florida or Abu Dhabi or the United Kingdom.”
Stopping Sepsis
The leading cause of death in hospitals is sepsis, a medical emergency that occurs when your immune system is overwhelmed with infection or overreacts to an infection and attacks your own organs. The most severe cases are cared for in the ICU. Led by Dr. Dweik, Dr. Khouli and critical care physician Vidula Vachharajani, MD, Cleveland Clinic is stepping up efforts to identify sepsis mechanisms and to diagnose and treat sepsis in its early stage, which will save lives.

Nurse Corey Large wraps up a 12-hour overnight shift. He graduated from nursing school in 2020. Since then, his career has been consumed by caring for patients with COVID-19. | Photo: Lisa DeJong
Endgame
Respiratory therapist Brittany Hanshaw, RRT, believes that she and her critical care colleagues will emerge from the pandemic with a newfound strength. “We’re already stronger because of everything we’ve had to deal with,” she says. “When this is over, COVID will have changed us for the better.”
For Hanshaw, the most rewarding part of her job is taking the breathing tube out of a patient and hearing their voice for the first time. “They’re so thankful that they’re alive,” she says. “They love to hear their own voice, too.”
Other voices fall silent forever.
“The hardest part is having to extubate someone to let them pass,” Hanshaw says. “Normally, a nurse comes in the room with us, and a doctor will be in the room or right outside. The respiratory therapist pulls the tube, but other caregivers are right there. It can be very draining, but we’re all there for each other.”
With support from Cleveland Clinic’s Caregiver Catalyst Grants program, which pools philanthropic gifts to fund the best and brightest ideas submitted by Cleveland Clinic caregivers, Smith created the Lavender Lounge. It’s a private space where caregivers can grieve a patient’s death, complete with soothing art on the walls and calming music in the background. “The room provides a respite for everyone,” Smith says, “every single day.”
Part of a wall in the MICU is covered with colorful paper butterflies. Each butterfly represents a patient who died over the past year. A couplet from poet Emily Dickinson — Unable are the Loved to die/For Love is Immortality — is surrounded by dozens and dozens of butterflies.
“A common conversation among critical care physicians is the need for patients to have either advance directives or clear discussions with their loved ones about what to do — before they come to us,” says Dr. Mireles-Cabodevila. “Obviously, we love pushing patients through and seeing them get better. At the same time, you can’t do anything else for some patients. Under those circumstances, there are a fair amount of end-of-life discussions and decisions to be made about helping patients die peacefully and with dignity. Every time you’re on a shift, it’s not without one of those discussions or one of those decisions.”

“Our ICUs don’t operate in a silo or in a vacuum. We have the ability to coordinate across our different ICUs, leverage their strengths and share resources.”
— HASSAN KHOULI, MD | Chair of Cleveland Clinic’s Department of Critical Care Medicine
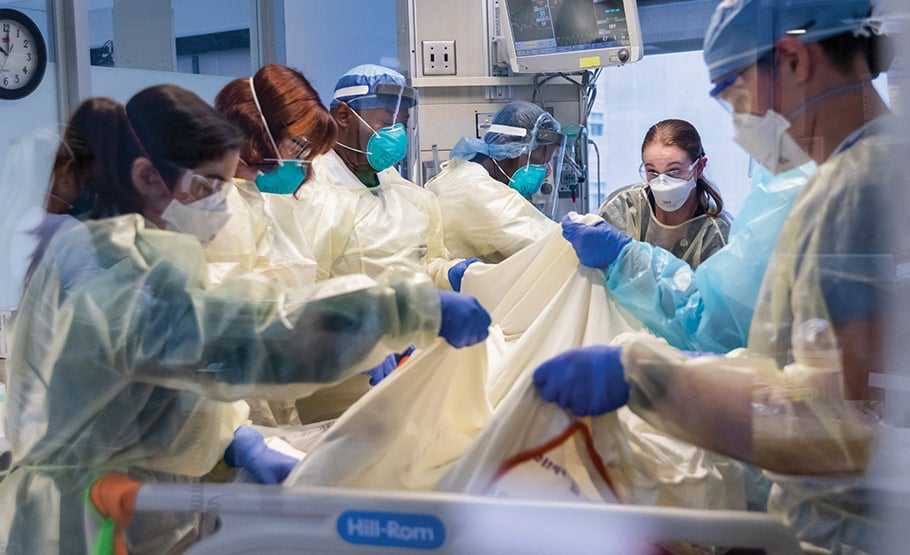
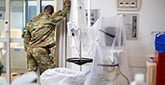
Caregivers work in concert to turn a patient to improve their breathing. A physician supervises the procedure. | Photo: Annie O'Neill
The Shape of Critical Care to Come
Critical care leaders at Cleveland Clinic have seen the future of the ICU, and it’s less invasive and more data-driven.
“The trend in our intensive care units is moving toward less invasive interventions,” Dr. Khouli says. “In some cases, that means no more breathing tube down the throat. When appropriate, we can deliver breathing support from the same machine with a face mask, without making the patient uncomfortable.”
Another case in point: point-of-care ultrasound. Advances in this technology have been a game-changer in hemodynamic monitoring, which charts the flow of blood through the cardiovascular system. Previously, this entailed inserting a catheter into a patient’s heart and arteries. With the high-resolution imaging provided by point-of-care ultrasound, caregivers can have a proverbial look inside, noninvasively.
“Every intervention that we do has potential side effects,” Dr. Dweik says, “which we like to avoid if we don’t have to put the patient through it.”
Big data also promises to play an increasingly crucial role in the ICU.
“The proliferation of electronic health records has generated a massive amount of data,” Dr. Khouli says. “It’s somewhat unstructured, and our teams have to navigate all this data on a daily basis. Where we’re heading is more toward artificial intelligence, informatics and machine learning, to leverage the data and structure it in a way that provides real-time information that we can act on.”
He adds: “These will be valuable tools, but they’ll never replace the brains of our multidisciplinary teams — or their human touch.”
Smith started her career as a critical care nurse in the MICU at Cleveland Clinic. Twelve years later, she’s still there. At the intersection of Life and Death, she knows that even the littlest acts of kindness go a long way.
“Any person in any one of those beds could be one of my family members — and how would I want my family member treated?” she says.
“You might not know anything about them. Perhaps they have no visitors. But they’re still a person; they’re very sick; and they need someone to provide some comfort. What draws me to this job is being able to brush their hair or brush their teeth or wash their face, things I can do for them that they can’t do for themselves. Make them look nice, even if they’re unconscious, because if they look nice, maybe they feel a little better. The sicker the patient is, the more they need those things.
“We’re their spokesperson when they can’t speak. We’re their advocate when they can’t advocate for themselves. We’re here to take care of everything.”
About the Photos
The powerful images that accompany this story were captured by Cleveland Clinic photographers Lisa DeJong and Annie O’Neill. They embedded themselves in MICU units G61and G62 on Cleveland Clinic’s main campus in late December 2021 and early January 2022, as critical care teams found themselves on the front lines of another COVID surge.
Wanted: Difference Makers
“As critical care continues to evolve, philanthropic support is essential,” Dr. Dweik says. The big data that will drive better care in ICUs requires world-class data scientists — and your gift will help Cleveland Clinic build a world-class team. Philanthropy also is needed to fund research that will deepen our understanding of sepsis, COVID-19 and other diseases. Supporting critical care at Cleveland Clinic means supporting the teams that care for the sickest of the sick and improving outcomes for patients in ICUs.
To learn more, call 216.444.1245 or send an email with “Critical Care” in the subject line to giving@ccf.org.